Liver is the largest solid Organ of our body, and it perform 100s of functions. It is the key organ in Glucose, Protein & Fat Metabolism. Living with diabetes already demands your attention, daily blood sugar checks, medication routines, meal planning, and lifestyle choices. But what if there’s something even quieter than high sugar, something happening inside your body that you won’t feel until it’s too late? That “something” is Fatty Liver Disease, now more accurately termed MASLD: Metabolic dysfunction-associated steatosis liver disease. And if you have Type 2 Diabetes, there’s a 2 in 3 chance your liver may already be affected. Let’s understand it simply, what it is, why it matters, and how to act early.
Defining MASLD (Previously NAFLD)
For years, this condition was known as NAFLD (Non-Alcoholic Fatty Liver Disease) which simply meant a fatty liver not caused by alcohol. But this term was misleading. It defined the disease by what it wasn’t instead of what it was. MASLD places focus where it belongs: on metabolic dysfunction, the very core issue in diabetes, obesity, and insulin resistance. It signals a broader, more accurate understanding of how fat builds up in the liver and what it means for overall health.
- MASLD is diagnosed when there is >5% fat in liver + one metabolic risk like
- Type 2 Diabetes / Prediabetes
- Overweight or Obesity
- High Cholesterol
- High Blood Pressure
- Unlike alcoholic liver disease, MASLD is caused by metabolic dysfunction, not alcohol.
- It affects up to 60–70% of people with Type 2 Diabetes and may even precede diabetes in some cases.
Why People with Diabetes Should Be Concerned
The statistics are sobering:
- 60% to 70% of people with Type 2 Diabetes have MASLD
- It may develop before diabetes and worsens it
- MASLD increases risk for:
- Liver cirrhosis
- Liver cancer
- Cardiovascular disease (the #1 cause of death in diabetics)
- Certain cancers and premature mortality
It’s often silent in early stages. No pain. No fatigue. No symptoms. By the time it speaks, your liver may already be damaged.
How MASLD Develops: A Metabolic Domino Effect
Fat doesn’t accumulate in the liver overnight. It’s a gradual process, often fueled by
- Consuming high-sugar or refined carbs, high-fat caloric loaded diet, Ultra-processed food – Most important factors.
- Overweight and obesity
- Sedentary lifestyle
- Chronic insulin resistance, which impairs fat metabolism
- Inflammation and oxidative stress damaging liver cells
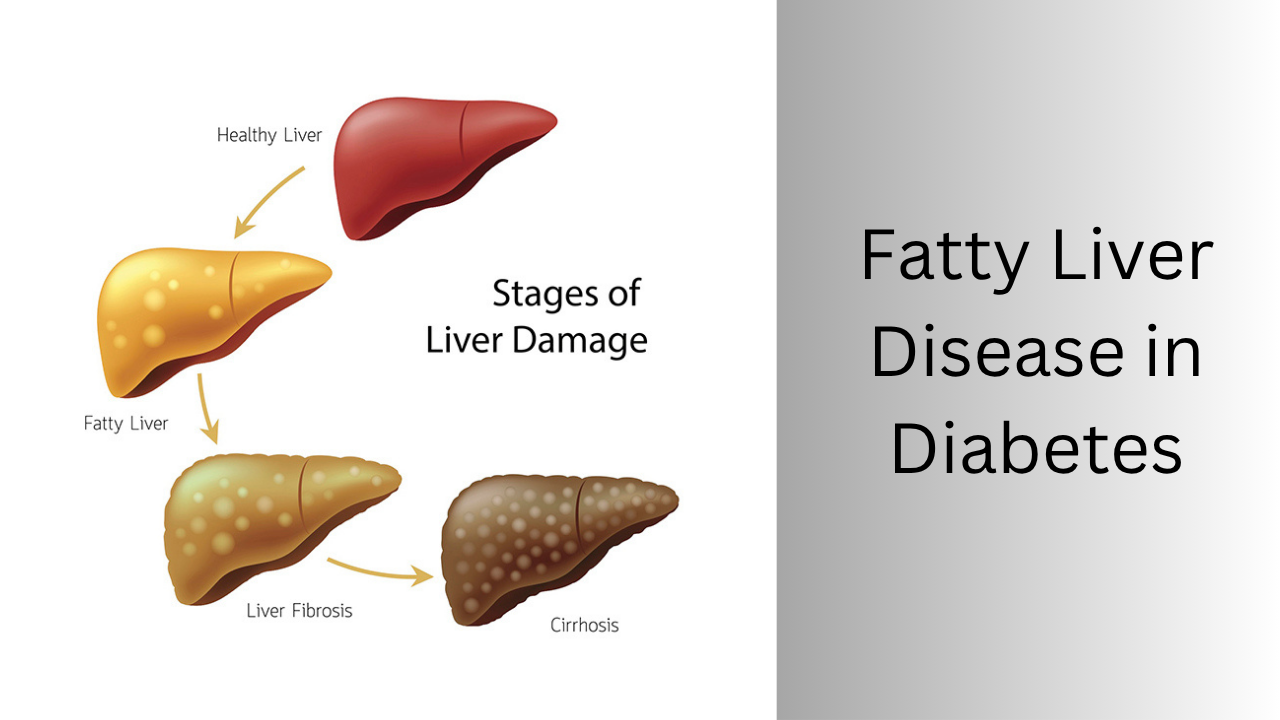
Over time, the liver goes from steatosis (simple fat accumulation) to fibrosis (scarring), and eventually to cirrhosis or even liver cancer.
The Spectrum of MASLD
Like diabetes, MASLD progresses through stages:
- Simple steatosis – fat in the liver, no inflammation
- MASH (Metabolic dysfunction-associated steatohepatitis) – fat plus inflammation and cell injury
- Fibrosis – early liver scarring
- Cirrhosis – advanced scarring, irreversible in late stages
- Hepatocellular carcinoma – liver cancer
But here’s the good news: the earlier you detect it, the greater your chances of full reversal.
Diagnosing MASLD: Don’t Wait for Symptoms
Diagnosis starts with awareness. If you have diabetes, prediabetes, or obesity, you should be screened. The diagnostic tools we use are:
- Liver function tests (ALT, AST) – May be normal even in advanced stages
- FIB-4 score – A simple online calculator using age, AST, ALT, and platelets to estimate fibrosis risk.
- Ultrasound (USG) – Detects fatty changes, grades liver fat from 0 to 3
- Fibro Scan – Measures liver stiffness; painless and non-invasive
- MRI or MR Elastography – Gold standard for quantifying liver fat and fibrosis
A FIB-4 score above 1.3, or liver enzymes 2–3x normal, should prompt consultation with a liver specialist or gastroenterologist.
Who Should Be Screened? Get yourself screened if you have Type 2 Diabetes or Prediabetes with overweight or obesity, or with high cholesterol or triglycerides or mild liver enzyme elevation, or ultrasound changes.
Treating MASLD: Start with Lifestyle, Always
There is no magic pill for fatty liver. But there is a powerful medicine that works almost every time: weight loss.
- Losing just 5% of body weight can reduce liver fat
- A loss of 10% or more can reverse steatohepatitis and reduce fibrosis
Lifestyle essentials:
- Eat better – Mediterranean-style diets work best:
✅ High in vegetables, nuts, olive oil, fish
❌ Low in processed carbs, sugar, and saturated fat - Move more – 150 minutes/week of exercise (brisk walking, strength training) improves insulin sensitivity and liver function
- Avoid alcohol – Even small amounts can accelerate liver damage
Lifestyle changes can reverse MASLD in many cases.
Treatment-Medical Therapies: More Hope Than Ever
Some diabetes medications also support liver health:
- GLP-1 receptor agonists (e.g. Liraglutide, Semaglutide) – Promote weight loss, reduce inflammation
- GLP1 + GIP agonists (e.g. Tirzepatide) – A dual-action therapy showing promising liver benefits
- SGLT2 inhibitors – Aid in glucose control and fat reduction
- Pioglitazone – Improves liver histology in some cases
- Resmetirom – A new liver-specific drug approved for MASH
These are not magic fixes but add-on tools, especially effective when combined with lifestyle changes.
Bariatric or Metabolic Surgery: When Nothing Else Works
For individuals with:
- BMI over 35
- Poor response to medications or lifestyle changes
Metabolic or bariatric surgery may offer a life-saving solution.
It not only improves diabetes and weight but also reverses liver fat and inflammation in many patients.
So, if you have Type 2 Diabetes, keep a watch on your Liver and discuss with your treating doctor before it is too late .