What is Continuous Glucose Monitoring (CGM)?
Continuous Glucose Monitoring, or CGM, is a system that helps people, especially those with diabetes, track their blood sugar (also called blood glucose) in real time all day and night. First introduced in the late 1990s, early CGMs were bulky and limited in accuracy. Over the past two decades, CGM systems have evolved significantly, becoming smaller, more accurate, and user-friendly. Today, CGMs are widely used in diabetes care, integrated with smartphones and insulin pumps, empowering individuals to make informed decisions for better glycemic control.
A small device is worn on the body, usually on the back of the upper arm or the stomach. This device checks blood sugar levels automatically every 1 to 5 minutes, giving between 288 and 1440 readings per day. With CGM, you can see your blood sugar level anytime and track how it changes over hours or days. This helps identify patterns, take corrective actions, and manage diabetes more effectively. Compared to traditional finger-prick blood sugar meters, CGM provides much more data and a clearer picture of your glucose trends.
Who can use CGM?
- People with Type 1 diabetes: CGMs are beneficial for those with Type 1 diabetes, as they help manage insulin dosages and identify potential hypoglycaemic (low sugar) or hyperglycaemic episodes ( high sugar).
- People with Type 2 diabetes: CGMs can also be beneficial for some individuals with Type 2 diabetes, especially those on insulin or who have difficulty controlling their blood sugar levels or who want to reverse their diabetes, if possible, with guided and supervised lifestyle measures (diet and exercise).
- People with Prediabetes: CGM can be an extremely beneficial tool to prevent diabetes in people with prediabetes. By using CGM, they can track their sugar levels in response to various types of food. They can make necessary changes in their diet and exercise regimen to maintain sugar levels in the normal range and prevent diabetes, as well as reverse the prediabetic condition.
- Pregnant Females with Type 1, Type 2, and Gestational Diabetes: Continuous Glucose Monitoring (CGM) is highly beneficial for pregnant women with Type 1, Type 2, or gestational diabetes. It provides real-time glucose trends, helping maintain tight glycemic control, reducing the risks of complications for both mother and baby. CGM supports timely dietary, medication, and insulin adjustments and better outcomes during this critical period.
- As a Biohacking Tool: Some individuals without diabetes are using CGMs as a lifestyle biohacking tool to gain insights into how their bodies process different foods and respond to physical activity.
Benefits of Using a Continuous Glucose Monitor (CGM):
Using a CGM can significantly improve diabetes management and overall health. Here are some key benefits:
- Continuous Monitoring: CGMs provide real-time glucose readings every few minutes, day and night, giving a complete picture of your blood sugar levels.
- Fewer Finger Pricks: Because the device continuously tracks glucose, you don’t need to do as many painful finger-stick tests.
- Trend Tracking: CGMs show how your blood sugar changes over time, helping you spot patterns related to meals, exercise, stress, or medication.
- Alerts and Alarms: The device can notify you immediately if your blood sugar goes too high or too low, helping you prevent dangerous situations.
- Better Decision Making: With more detailed information, you can adjust your insulin, food intake, or activity levels more effectively.
- Remote Sharing: Many CGM systems allow you to share your glucose data with healthcare providers or family members, providing extra support and safety.
- Improved Health Outcomes: Using a CGM helps maintain better blood sugar control, which can lower the risk of diabetes-related complications and improve your overall quality of life.
- Peace of Mind: Knowing your glucose levels at all times reduces anxiety and gives you confidence in managing your condition.
Is CGM different from BGM?
CGM (Continuous Glucose Monitoring) and BGM (Blood Glucose Monitoring) are both used to track blood sugar levels, but they work differently. BGM requires a finger-prick blood sample and gives a single reading at that moment. CGM, on the other hand, uses a small sensor placed under the skin to check glucose levels every few minutes, providing real-time data and trends throughout the day and night. While BGM is more accurate for spot checks, CGM offers more convenience, alerts for highs and lows, and a better overall picture of the trend showing how blood sugar changes over time.
CGM Devices available in the UAE at present
The devices available in the UAE at present are- Free Style Libre 2 Plus, Dexcom 7, Sibionics, Intelligo etc.
How to Interpret and Analyse CGM Data
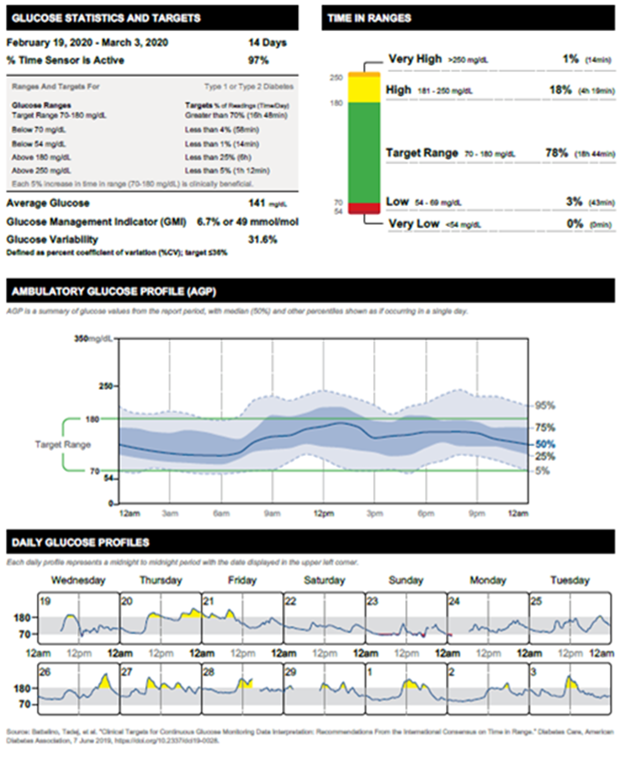
CGM is helpful only if you know how to interpret and analyse data. It is a continuous learning tool, but you must know how and what to learn to improve your diabetes. Key metrics include Time in Range (TIR), which shows the percentage of time glucose levels stay within target (usually 70–180 mg/dL); Time Above Range (TAR) and Time Below Range (TBR), indicating hyperglycaemia and hypoglycaemia time and durations. Daily trend graphs help identify glucose patterns linked to meals, exercise, or stress, which helps in improving the lifestyle. The Coefficient of Variation (CV), a measure of glucose variability, should ideally be below 36% to ensure stable control. By regularly reviewing these insights, patients and clinicians can fine-tune treatment plans for safer, more effective blood glucose management. If you don’t learn to interpret, analyse, and draw conclusions from data, CGM may not help you much.
Tips for Getting the Most out of Your CGM
- Ensure Proper Calibration: Always wash your hands before performing a fingerstick for calibration. If washing isn’t possible, wipe away the first drop of blood and use the second drop. This helps avoid inaccurate readings due to contaminants.
- Be Patient with Day One Readings: CGMs tend to be less accurate during the first 24 hours after sensor insertion. To improve accuracy, consider inserting a new sensor 3–12 hours before your current sensor expires, a technique known as “soaking the sensor”.
- Avoid Calibration During Rapid Glucose Changes: Refrain from calibrating your CGM when your glucose levels are low or fluctuating rapidly, as this can lead to less accurate readings.
- Choose Compatible Devices: If your CGM readings don’t align well with your blood glucose meter, try using a different brand of good quality glucometer or CGM. Some devices may offer better compatibility and accuracy. Cross checking of CGM by good glucose meter is required off and on as some sensors may be faulty .
- Manage Alarms Effectively: Set your CGM alarms at conservative thresholds initially, such as 70 mg/dL for low and 250 mg/dL for high. Adjust these settings over time to minimize alarm fatigue while maintaining effective glucose monitoring.
- Understand Trend Arrows: Pay attention to trend arrows on your CGM. A rising arrow indicates increasing glucose levels, while a falling arrow suggests decreasing levels. This information can help you make timely adjustments to your insulin or carbohydrate intake.
- Be Cautious with Medications: Some medications, such as acetaminophen (Tylenol), can cause false high readings on specific CGM devices. If you take such medications, consider using a different CGM model or confirm readings with a blood glucose meter.
Conclusion
CGM offers a powerful way to monitor blood sugar continuously and make smarter decisions about your health. Whether you have Type 1 or Type 2 diabetes, Gestational diabetes, Prediabetes or want to understand your body better, CGM can be a game-changer. Talk to your healthcare provider to see if CGM is right for you.





